Health Information



Scaphoid Fracture
Common Wrist Injuries (II): Scaphoid Fracture
Mechanism of Injury
Injury usually occurs from falling on an outstretched hand.
Symptoms
Fractures are not always painful and often the patient can still move their wrists. Symptoms may include pain and tenderness over the scaphoid tuberosity and/or in the anatomical snuff box, as well as swelling and bruising.
Diagnosis
The diagnosis is usually confirmed with an x-ray, however sometimes a scaphoid fracture may not show up on x-ray for the first 1-2 weeks. An additional CT scan or MRI may be required to confirm the diagnosis or repeat x-ray 1-2 weeks later.
Referral
If the fracture is stable, the patient should be referred immediately for a custom made thermoplastic splint or cast.
If the fracture is unstable and requires surgery, early referral post-surgery or removal of the cast is a good practice.
Management
Scaphoid fractures can take a long time to heal depending on the nature and the location of the fracture. Blood flow to the scaphoid enters at the distal portion of the bone and there is no direct blood supply to the proximal portion of the bone. This retrograde blood supply is why proximal pole fractures are associated with the poorest union rates and the longest time to union.
Stable Fracture
- A custom made thermoplastic splint or cast is usually required for approximately 6-8 weeks but can be longer.
- Early oedema management and mobilisation of unaffected joints
- Personalised exercise program to regain wrist/thumb movement and strength after removal of the splint/cast
- Advice regarding precautions during the different stages of rehabilitation.
Post-Surgery
- A custom made thermoplastic splint is usually required for 6-8 weeks, sometimes longer
- Wound care including dressing changes and removal of sutures
- Early oedema and scar management to prevent stiffness
- Early mobilisation of the hand and wrist if stability allows
- Wrist and grip strengthening from 8 weeks post surgery
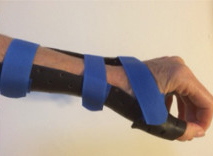
Splinting
A thumb spica splint or cast remains the most predominant style of orthosis used in clinical practice, however the inclusion of the thumb in a cast has not been shown to increase scaphoid union rates or accelerate time to union.
|
|
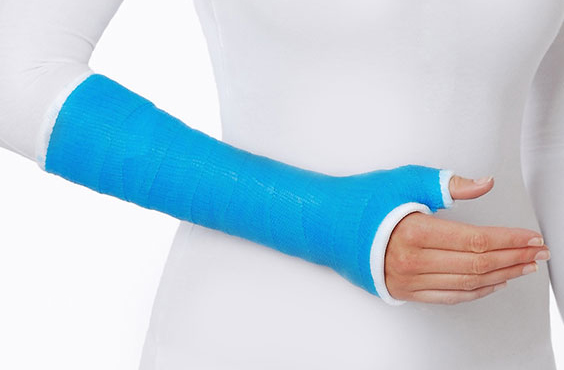
Casting
|
|